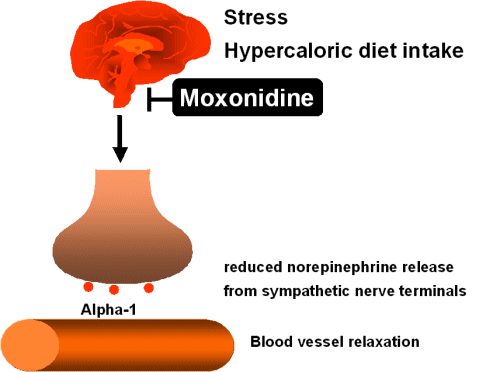
Moxonidine
reduces sympathetic outflow of the brain
Moxonidine interacts with imidazoline I1-receptors
in the rostroventrolateral medulla and thereby inhibits sympathetic
outflow of the brain. This area of the brain is involved in the
baroreceptor reflex which is important for adaptation of the body to
postural changes. For example, a reduced venous return to the heart
activates cardiopulmonary receptors leading to a rise in sympathetic
outflow. Unfortunately, this mechanism adjusts to long term changes in
blood pressure, i.e. baroreceptor resetting, and does not respond
anymore to a pathologically raised high blood pressure, i.e.
hypertension.
It appears that
moxonidine interacts with neurons within this pathway and thereby
reduces sympathetic outflow. However, no effects on postural reflexes
have been observed. If, however, lifestyle factors raise sympathetic
outflow of the brain, moxonidine appears to downregulate the
sympathetic activity by interfering with the medullar
centers involved in the baroreceptor reflex.
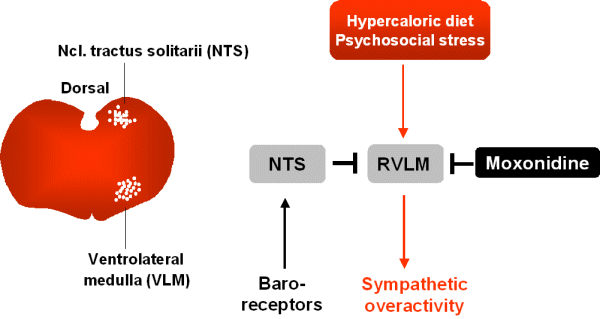
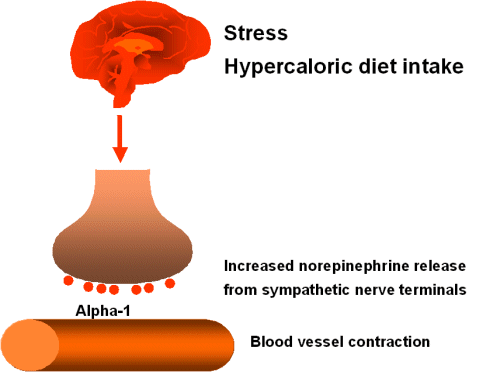
An increased sympathetic activity not only
results in
hypertension but also favours insulin resistance. The chain of events
is
shown for the example of hypertension which often is mediated by a
greater activation of peripheral alpha-1 adrenergic receptors:
A moxonidine-mediated reduction in the
sympathetic outflow
of the brain results in a smaller number of norepinephrine molecules
released
from sympathetic nerve terminals. Thus, there will be less
vasoconstriction due to reduced alpha-1 adrenoceptor effects. In
addition, various functions of the body such as insulin sensitivity are
expected to be affected in a beneficial manner.